Medical Credentialing Services
QuickMBS provides end-to-end medical credentialing solutions to help healthcare providers get enrolled with insurance payers efficiently. Our specialists manage the entire process — from application submission to approval — ensuring compliance, accuracy, and faster provider onboarding.
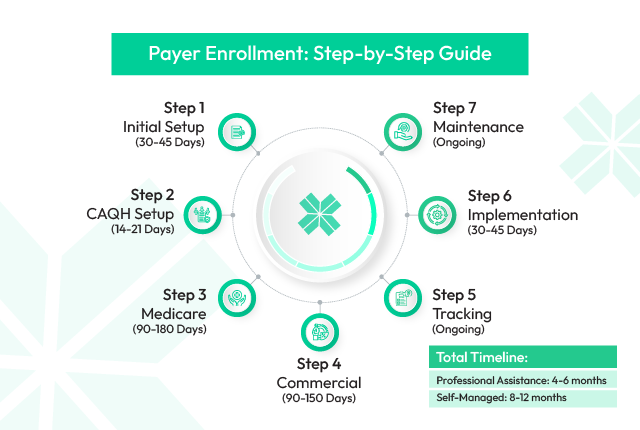
Provider Enrollment
We handle complete provider enrollment with commercial and government insurance payers, ensuring accurate application submission and faster network participation.

Insurance Network Contracting
QuickMBS assists providers in contracting with insurance networks, negotiating participation terms, and securing in-network status efficiently.

CAQH Profile Management
We create, update, and maintain CAQH profiles to ensure payer access to accurate provider credentials and reduce enrollment delays.
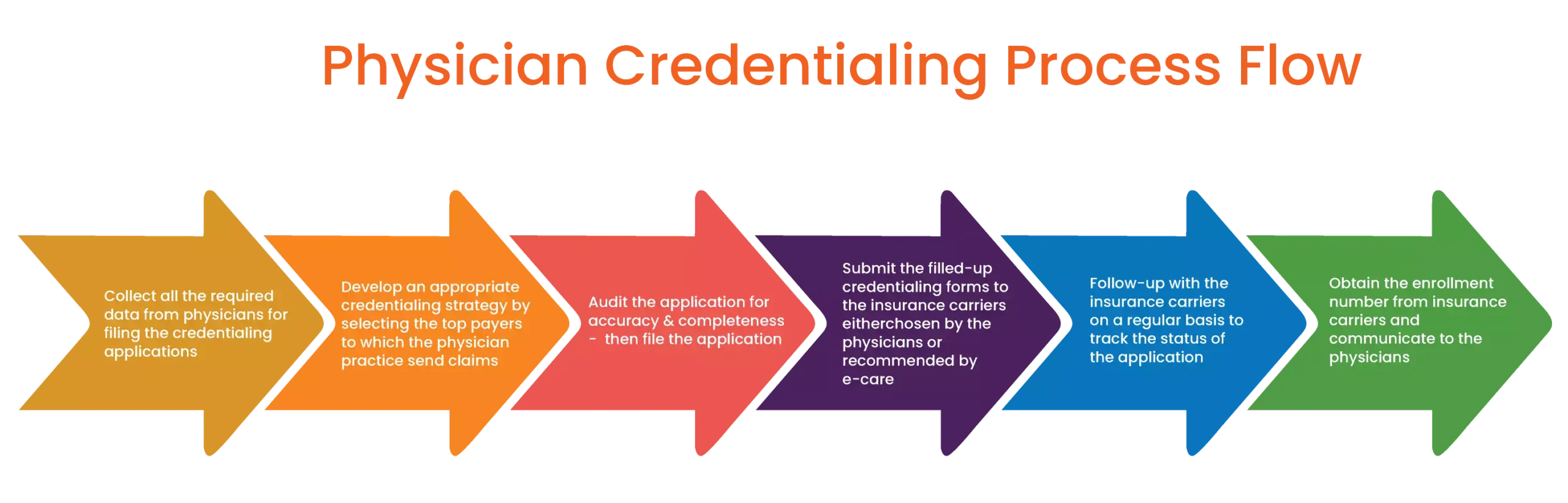
Credential Verification
Our specialists verify licenses, certifications, education, and work history to ensure full compliance with payer and regulatory requirements.
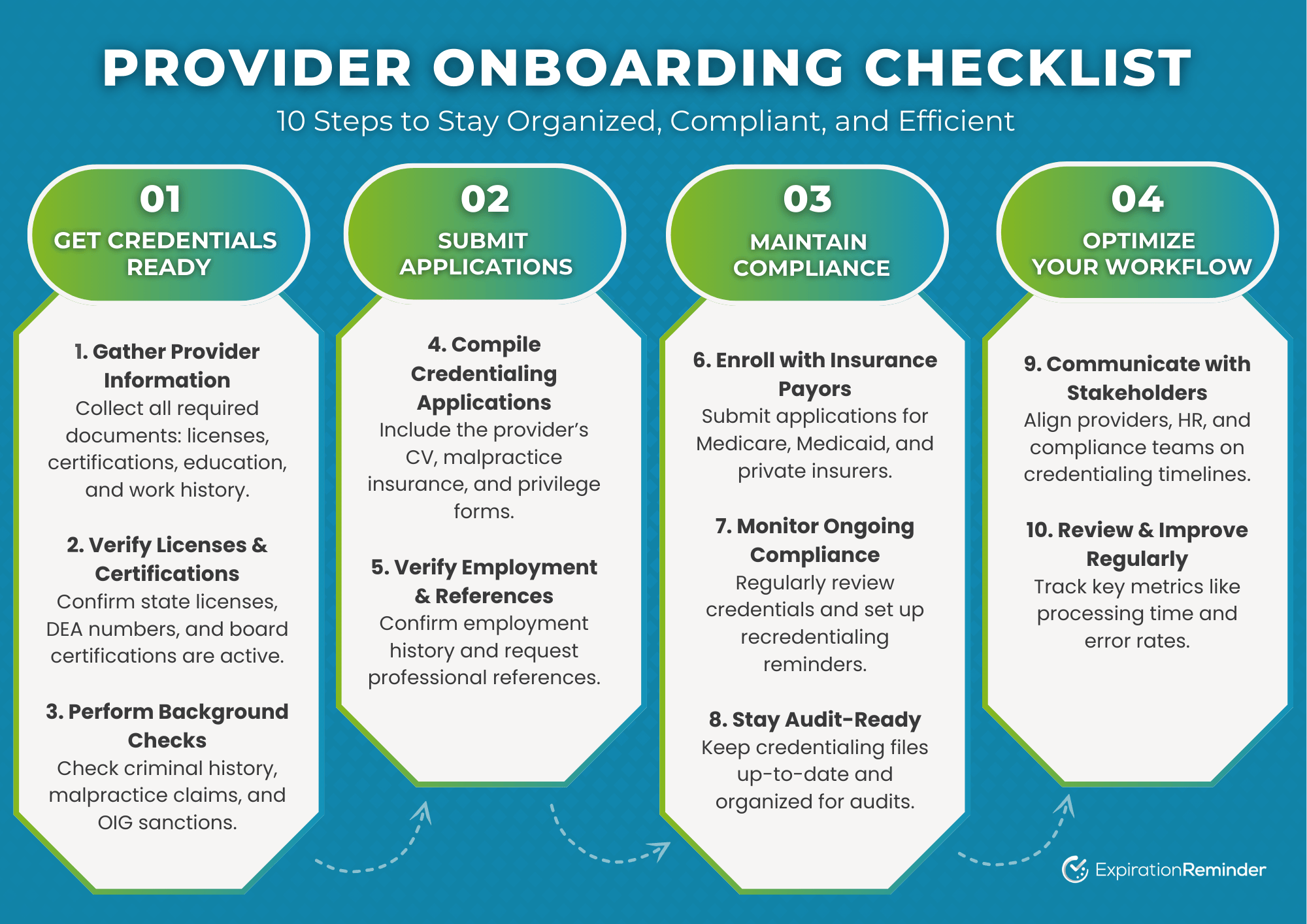
Re-Credentialing & Renewals
QuickMBS tracks expiration dates and manages re-credentialing to keep providers active within insurance networks without interruptions.

Hospital Privileging Support
We assist providers in obtaining hospital privileges by managing documentation, applications, and committee review coordination.

With access to
24 Hour
Emergency
Dediated Billing Assistance
QuickMBS supports healthcare providers with reliable billing solutions that ensure accuracy, compliance, and consistent revenue flow.
Service Recipient Says

“Their credentialing team handled documentation and payer follow-ups with precision, saving us valuable administrative time.”
Lisa Grant Practice Manager
“Thanks to QuickMBS, our providers were credentialed quickly, allowing us to begin billing without unnecessary delays.”
Dr. Ahmed Khan Multi-Specialty Clinic Owner




























“QuickMBS made our credentialing process seamless. We were enrolled with multiple insurance networks faster than expected.”
Dr. Jonathan Reeves Primary Care Physician